Currently, a large number of people suffer from osteochondrosis. Many of them don't even know about the existing problem. However, if you do not start treatment in time, complications will occur that will be felt for the rest of your life. Osteochondrosis, like many other diseases, "gets younger" and significantly worsens the quality of life, leaving it out of its usual rhythm.
In our article we will learn a little about the disease itself, as well as dwell in detail on the medical method of its treatment.
Osteochondrosis and its types
Osteochondrosis is a deformation of the articular cartilage, bone tissue of the spine and intervertebral discs.
Osteochondrosis happens:
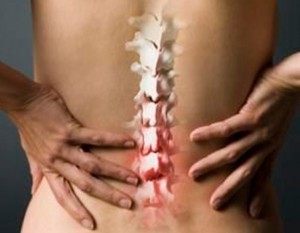
- lumbar (lumbosacral),
- cervical, chest
- .
Causes of osteochondrosis:
- upright walk,
- curvature of the spine,
- spinal injury,
- flat feet,
- frequent weightlifting,
- frequent changes in the position of the torso,
- prolonged stay in uncomfortable positions,
- column overload,
- physical inactivity and obesity,
- malnutrition,
- stressful conditions.
Stages of development of osteochondrosis
- Due to certain changes in the intervertebral disc, instability of the vertebrae appears. The spine is very prone to injury.
- The destruction of the fibrous ring of the intervertebral disc begins. The intervertebral gap narrows.
- The fibrous ring breaks. The pulpy nucleus of the intervertebral disc protrudes. Due to the formation of an intervertebral hernia, deformity of the spine is caused.
- A pronounced pain syndrome occurs. Due to the formation of bone growth and ossification of the spinal ligaments, movements become limited.
Symptoms of osteochondrosis
Lumbar region (lumbosacral)
- Back pain and constant pain.
- Sensation of pain and numbness in the limbs.
- Decreased physical activity.
- Increased pain when making sudden movements, lifting weights, exercising, sneezing and coughing.
Cervical region
- Pain in arms and shoulders, headaches.
- Vertebral artery syndrome (burning, throbbing headache, dizziness, noise in the head, colored spots and "flies" in front of the eyes).
Chest
- Pain in Organs internal organs, in particular in the chest ("stake" in the chest) and in the heart area.
Determining the diagnosis
The diagnosis is made in consultation with the neurologist based on the patient's complaints (painful syndrome, limited mobility, etc. ). The spine is examined by him in the patient's standing, sitting and lying position (at rest and in motion). When examining the back, attention is paid to posture, the structural features of the torso, the lower angles of the shoulder blades, the lateral contours of the neck and waist, the position of the shoulder straps, etc. Then, the doctor, as a rule, refers the patient for radiography, computed tomography or magnetic resonance, with which the diagnosis is clarified and made concrete, the degree of damage is determined and hidden deviations from the norm are revealed. Based on the data obtained, the neurologist prescribes the appropriate treatment. As a rule, it is a complex therapy, which includes the use of medications, massages, exercise therapy and other methods.
Therapeutic exercises for osteochondrosis of the lumbar spine
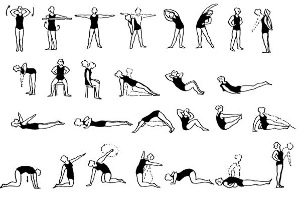
Treatment of osteochondrosis with medications
To begin with, it should be noted that in the early stage of development of osteochondrosis, in some cases, you can do without medication. It will be enough to use corrective gymnastics, applicators of all types, in addition to reducing loads and eliminating other causes of the disease. If symptoms are gaining strength and studies show characteristic changes, medications that help influence both the cause and symptoms of osteochondrosis should be used.
The treatment of osteochondrosis with medications is indicated during the period of its exacerbation and aims to relieve the inflammatory process, relieve pain and enhance the metabolic processes through internal intake or administration of injectable drugs.
As osteochondrosis is a systemic disease that negatively affects several organs and systems, its treatment must be comprehensive. Medicines for the treatment of osteochondrosis perform the following tasks:
- pain relief,
- removal of inflammation,
- improving blood circulation in the affected tissues,
- cartilage restoration,
- restoring joint mobility,
- elimination of depression caused by constant pain.
So, what medications can a neurologist prescribe to treat osteochondrosis?
- NSAIDs (non-steroidal anti-inflammatory drugs).
Eliminate inflammation and pain. They are used externally (gel, cream), internally (capsules, tablets), as well as in the form of injections (intramuscular, intravenous, subcutaneous).
- Vasodilators (vasodilators).
As a result of muscle tension and pain in osteochondrosis, blood vessels narrow. To avoid undesirable consequences in this context, the doctor may prescribe vasodilator drugs for a better restorative effect.
- Muscle relaxants (muscle relaxants).
Muscle relaxants have a relaxing and calming effect on your muscles. The healing process without drugs in this group is slower, because, due to its properties, blood circulation normalizes, the sensation of pain decreases, mobility returns and the affected tissues recover more quickly.
- Chondroprotectors.
Chondroprotectors no longer cause destruction, they stabilize the condition. Taking chondroprotectors is long term, for life, the effect occurs after treatment for a period of at least 6 months. Chondroprotectors are used externally, internally and in the form of injections.
- glucosamine
- chondroitin
- glucosamine + chondroitin
- glucosamine + chondroitin + vitamins
- Sedatives (sedatives).
Long-term pain syndrome can trigger stress and depression. In that case, valerian, fennel and combined herbal preparations are prescribed. For more serious disorders, antidepressants and hypnotics are used to improve the process of falling asleep and the quality of sleep.
- Vitamins and vitamin and mineral complexes.
B vitamins are of great importance here, as they are able to restore the sensitivity of the affected nerve fibers and reduce pain.
For the general strengthening of the body, vitamin and mineral complexes can also be prescribed.

























